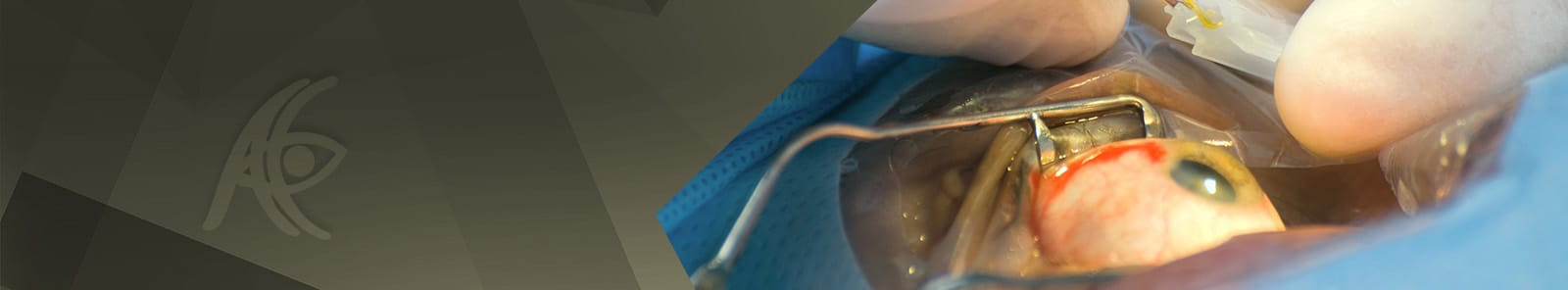
Cataract Surgery
Cataract surgery is probably the commonest surgery to be performed all around the globe, and also one of the safest. Once a cataract forms inside the eye, the only method to restore good vision is the surgical extraction of the cloudy lens. This is followed by the implantation of an artificial lens in its place that performs the function of the natural lens. Phaco-emulsification is the commonest method of cataract surgery. Explained below are the various techniques of surgery and the different types of lenses available for implantation.
Phaco-emulsification

This is a technique by which the cataract is liquefied and removed from inside the eye by a special equipment known as the Phaco-emulsification unit. The actual operation is carried out through a 2.8mm incision with the help of a titanium needle vibrating at the rate of about 40000 times per second. The needle emulsifies the cataract which is then aspirated.
Earlier, cataract surgery was performed through an incision as large as 10-12mm. Phaco has reduced this size drastically to 2.8mm. This eliminates the need for stitches as the wound is small and self-healing. Also, phaco reduces the risk factors associated with surgery, decreases the recovery time with early vision stabilization, and helps in reducing the surgically induced astigmatism.
Micro-incision Cataract Surgery
Also referred to as MICS, is a superior form of Phaco-emulsification in which the incision size is further reduced to a mere 1.6-1.8mm. The surgery is carried out by the Stellaris Phaco-emulsification system. It offers greater safety at the time of the surgery with reduced risk of intra-operative complications. The micro-incision means much less discomfort after surgery and quick post-operative recovery. Because the incision is so small, the astigmatism induced is almost nil.

Rigid Lenses
These are the conventional intra-ocular lenses. They are made up of a special material called PMMA (Polymethyl methacrylate). Rigid lenses have been in use for a long time but are now being gradually replaced by foldable lenses because of a few drawbacks. As the name indicates, they are rigid in nature, and so, a larger incision of 5.2mm is required for their insertion as compared to 2.8mm for foldable lenses. This increases the risk of post-operative endophthalmitis, delays wound healing and increases the surgically induced astigmatism. Also, glare experienced by patients, especially at night, is significantly greater. Such lenses are now seldom used in the developed world.
Foldable Lenses
 These are a step above the conventional rigid lenses. They are made up of a special optical material that, as the name suggests, is foldable in nature. This allows the surgeon to “fold” the lens on itself and insert it inside the eye through a smaller incision with the help of a special instrument, the injector. The smaller incision offers the patient many advantages including less trauma, faster recovery, minimal post-operative astigmatism and less chances of infection.
These are a step above the conventional rigid lenses. They are made up of a special optical material that, as the name suggests, is foldable in nature. This allows the surgeon to “fold” the lens on itself and insert it inside the eye through a smaller incision with the help of a special instrument, the injector. The smaller incision offers the patient many advantages including less trauma, faster recovery, minimal post-operative astigmatism and less chances of infection.
Another major advantage of foldable IOLs is less glare, especially at night time. The larger size of these lenses allows a more uniform refraction of light. On the other hand, patients with rigid lenses might experience some glare, more so, with direct light. This is due to their smaller optical size which may cause irregular refraction of light from the edge of the lens.
Aspheric Lenses
Aspheric lenses are an advanced type of foldable lenses. They are aberration free. With advancing age, aberrations develop in the cornea of the eye which diminish the quality of vision in dim light. Such changes are neutralized by aspheric lenses and, hence, the latter improve the quality of vision at night time.
Hydrophobic Lenses
As the name indicates, these lenses are made up of a material that does not “attract” water. The advantage is that they are associated with a lesser incidence of posterior capsular opacification (see “Yag Laser Capsulotomy” below) after cataract surgery. This makes these lenses suitable for children and those with intraocular inflammatory conditions.
Multifocal Lenses

Multifocal lenses go a step further than the above mentioned intra-ocular lenses by overcoming a major drawback of theirs. They allow for near vision in addition to vision for distance, hence, allowing the patient to be considerably independent of glasses even for near work.
These lenses are based on a principle, somewhat similar to that of bifocal spectacles. Bifocals help a person for near as well as distance as they incorporate both glass powers in the same lens. The same is true for multifocal IOLs, the difference being that the latter are ‘multifocal’ instead of ‘bifocal.’ These lenses are made up of rings of gradually varying powers that allow for appropriate focusing of light rays from objects at varying distances.
Multifocal lenses, too, are foldable in nature and, hence, can be inserted through a small incision of only 2.2mm.
Some patients might experience a mild visual discomfort after multifocal lens implantation, such as the appearance of fine rings in the visual field. These usually disappear after the other eye is operated upon and a similar lens inserted. This balances the visual mechanism in both eyes. For this reason, patients opting for multifocal lenses are advised to get their other eye operated upon as soon as possible, usually within a month of the first. Also, it is to be mentioned that though multifocals help for near vision as well, glasses may be required for very fine work.
Micro-incision Lenses

Micro-incision lenses or MILs are the latest generation of unifocal lenses to be introduced. Their main quality is the ability to be inserted into the eye through an incision as small as 1.8mm. The patient is operated upon by a more advanced form of phaco-emulsification called MICS or Micro-incision Cataract Surgery. The greatly diminished wound size results in superior post-operative comfort and a much faster recovery as compared to regular phaco-emulsification where other lenses are implanted. In addition, all the advantages of aspheric lenses are provided by MILs.
Toric Lenses
These are an advanced form of intra-ocular lenses, used in patients with high degrees of astigmatism.The residual post-operative astigmatism is significantly reduced as compared to situations in which other forms of lenses are used.
Accommodative Lenses
These intra-ocular lenses have been introduced with a new concept of restoring near vision by simulation of the normal process of accommodation that takes place inside the eye. When one looks at a near object, the eyeball tries to increase its focusing power by increasing the power of the crystalline lens. This aids in clear near vision. When this crystalline lens is removed after cataract surgery, problems tend to arise with near vision due to the inability to accommodate. Accommodative lenses tend to simulate the normal crystalline lens in this respect, and thereby help in clear distance as well as near vision.
Yag-Laser Capsulotomy

The natural lens has a cellophane like outer lining called the capsule. During cataract surgery, the back membrane of the lens, the posterior capsule, is left in place to support the artificial lens implant. The posterior capsule is normally clear and transparent. However, a majority of the people who undergo cataract surgery eventually develop a haziness or thickening of this membrane. Also referred to as “After Cataract,” this may develop months to years after the surgery. It is treated by a procedure called Yag Laser Capsulotomy, whereby the doctor uses a laser beam to make an opening in the posterior capsule to allow light to pass through and allow clear vision. This is a painless, out-patient procedure and never a part of the original cataract operation.