What is Corneal Blindness?
The cornea is the eye’s outermost layer. It is the clear, dome-shaped surface that covers the front of the eye. When this cornea becomes cloudy, light cannot penetrate the eye to reach the light-sensitive retina, resulting in poor vision or blindness.
After cataracts, glaucoma and age-related macular degeneration, corneal eye disease is the most common cause of blindness. It affects more than 10 million people worldwide.
What is a Corneal Transplant?
Corneal transplant, also known as keratoplasty, is a surgical procedure where a damaged or diseased cornea is replaced by donated corneal tissue. It is the most commonly performed organ transplant procedure, worldwide. When the entire cornea is replaced it is known as penetrating keratoplasty, and when only part of the cornea is replaced it is known as lamellar keratoplasty.
Who needs a Corneal Transplant?
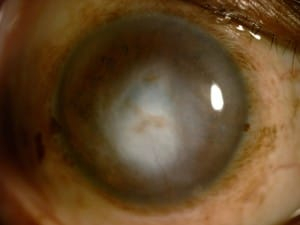
As an unhealthy and unclear cornea cannot give us the essential vision that we require, a transplant is required. An ideal candidate for the transplant is the one who:
- Has damaged cornea either due to some eye disease/infection or eye injury.
- Has keratoconus-where the cornea shape changes and becomes pointed, thereby affecting the vision grossly.
- Corneal scarring
The Surgical Procedure
The patient is either given general anesthesia, or local anesthesia and a sedative. The eye to be operated is then draped. An eyelid speculum is placed to keep the lids open, and some lubrication is placed on the eye to prevent drying of the eyes. The surgeon then uses a special circular cutting instrument called a trephine to remove a round section of damaged cornea from the front of the eye.
The same process is used to remove a similar-sized circle of cornea from the donor’s eye. The surgeon places the new section of cornea onto the recipient’s eye. The recipient’s eye is then stitched under the microscope. The eye is then patched after instilling antibiotic eyedrops till the anesthesia effect wears off. Following this, the patient is discharged and called next day for the first postoperative appointment.
Types of Corneal Transplants
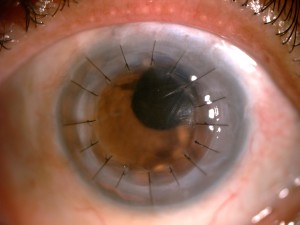
Since, the cornea contains five layers. Cornea transplants don’t always transfer all the layers. The different types include the following:
Penetrating Keratoplasty: In this the entire cornea (comprising of all layers) is replaced with the donor.
Lamellar Keratoplasty: This procedure selectively replaces diseased layers of the cornea while leaving healthy layers in place.
Deep anterior lamellar keratoplasty (DALK): In this procedure, the anterior layers of the central cornea are removed and replaced with donor tissue. Endothelial cells and the Descemets membrane are left in place. This technique is used in cases of anterior corneal opacifications, scars, and keratoconus.
Descemet’s Stripping Automated Endothelial keratoplasty (DSAEK): This is a highly refined technique that replaces just the endothelial layer of the cornea, allowing the specific cause of the patient’s vision loss. Since, no sutures are used in this technique, recovery of the patient is much faster.
Success after a Corneal Transplant
Corneal transplant are the most successful of all the transplants. Most people have a good vision for many years. Though, one may need glasses or contact lenses to achieve the best vision. Rigid gas permeable contact lenses, also known as RGP or GP lenses, and hybrid contact lenses usually are the most suitable contacts for corneal transplant patients due to the irregularity of the cornea after transplant. Laser vision correction may also be explored if you have nearsightedness, farsightedness, or astigmatism after the transplant has fully healed.
Corneal Graft Rejection
Though, corneal rejection is uncommon but, it may occur. However, if detected well in time, it can be treated and reversed in most circumstances.
Risks associated with a Corneal Transplant
- Infection
- Raised pressure inside the eye (Glaucoma)
- Rejection
- Graft Failure

