Glaucoma is a condition of the eye in which the pressure inside it increases beyond a level, such that it starts damaging the optic nerve. This is not a very uncommon condition and affects approximately 1% of the adult population above the age of 40 years, making it one of the most common causes of irreversible visual loss in the population. As much as 12% of the blind population of USA and UK is due to glaucoma.
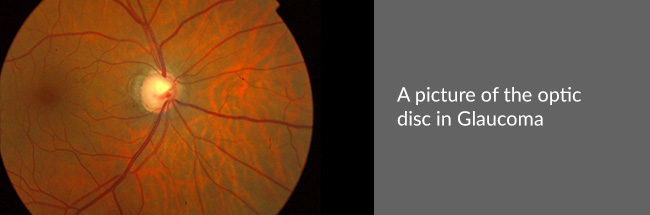
Explanation
Our eyes are filled with a fluid called aqueous humour. It is continuously secreted inside the eye, as well as drained from it. This fluid maintains a pressure inside the eye called the intra-ocular pressure or IOP. A critical balance is maintained between inflow and outflow of aqueous so that the IOP remains within normal limits. Due to any reason when the IOP becomes elevated, it may start damaging the optic nerve. If uncontrolled, this condition may slowly progress to blindness.
Risk factors for Glaucoma
- Advancing age – It is commoner in the elderly population, usually 40yrs or above.
- Race – It is commoner and more severe in blacks.
- Family history of glaucoma – especially in a first degree relative.
- Elevated intra-ocular pressure.
- Myopia – The optic nerve in myopes is more susceptible to damage, sometimes even at normal intra-ocular pressures.
- Diabetes
- Hypertension
Symptoms

Glaucoma can be regarded as a silent killer. The visual loss associated with this disease is slow, progressive and not associated with any objective symptoms. Due to optic nerve damage, loss of a person’s visual field starts slowly from the periphery and progresses towards the centre. As a result, a person may be unaware of the condition. This is exactly the scenario in our country where many patients present late, when as much as 40% of visual field loss has already occurred.
Treatment
The treatment of glaucoma is essentially aimed at controlling the elevated intra-ocular pressure. A host of medications are available for this purpose, in the form of eye-drops. Depending upon a patient’s condition, a single drug or their combinations may be required.
Things to remember while instilling anti-glaucoma medication
- Wash your hands before the procedure.
- Shut your eyes after instillation for about 5 minutes and at the same time for about 2 minutes press the inner angle of the eye with the index finger. This diminishes the drainage of the drug and allows maximal drug delivery to the eye.
- Wash your hands after the procedure.
- Instill your medications at a specific time everyday.
Sometimes, patients may require surgery if the IOP cannot be controlled medically, or for other reasons. This procedure is called Trabeculectomy. The main aim of this procedure is to drain the aqueous humour from the eye, into a space called the sub-conjunctival space. The additional outflow tract created automatically lowers the pressure inside the eye.
Facts about Glaucoma Treatment
- As a disease, glaucoma can be compared to diabetes – it can only be kept under control and cannot be cured. So, it is imperative that a patient takes his medication regularly so that the I.O.P. remains within normal limits.
- The visual field loss due to glaucoma is permanent and irreversible. Treatment is mainly directed to prevent further damage and preserve the patient’s existing vision.
- Some patients may develop an allergy to the anti-glaucoma drugs being used. They may develop redness, watering or irritation. This does not affect vision and merely requires the use of an alternative drug.
Investigations that maybe required in Glaucoma
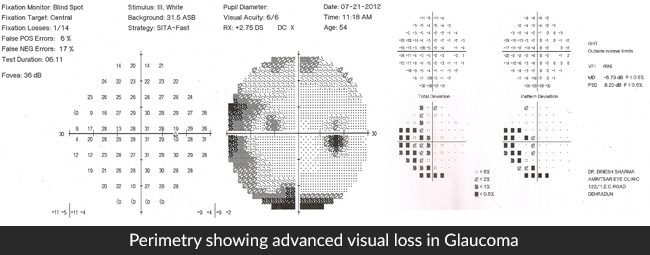
Perimetry – It is a computerized assessment of a person’s visual field.
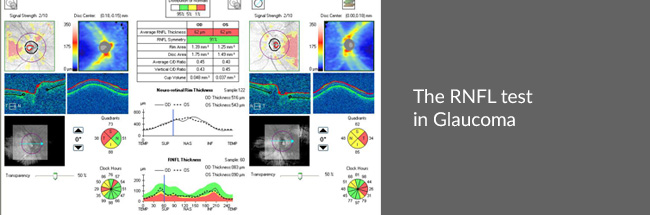
Retinal Nerve Fibre Layer (RNFL) test – It involves a detailed analysis of a person’s retinal nerve fibre layer at a microscopic level to ascertain the condition of the optic nerve and the extent to which it is damaged by the glaucomatous process.
Optic Disc Analysis – a detailed analysis of the optic disc is done by the OCT machine which is also used to do the RNFL test.
Follow Up
All patients of glaucoma require a regular ophthalmic check-up, at least once in 3 months. If the disease is advanced, the follow-up may be more frequent. It is also recommended that the glaucoma investigations be repeated at least every 6 months.

